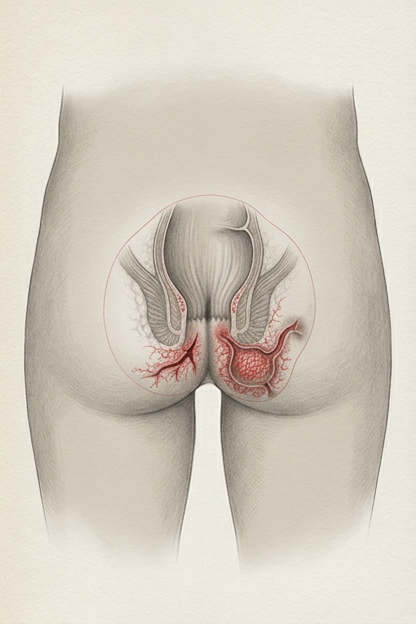
A chronic inflammatory bowel disease
that affects all layers of the digestive tract
Crohn's disease is an autoimmune condition and, along with ulcerative colitis, is a type of Inflammatory Bowel Disease (IBD). Crohn's disease is an inflammatory bowel disease where inflammation occurs throughout the entire digestive tract, from the mouth to the anus, and affects all layers of the bowel wall. It primarily occurs in the duodenum, small intestine, and large intestine, and clinical symptoms vary depending on the site of inflammation.
Unlike ulcerative colitis, where inflammation is limited to the mucosa and submucosa, in Crohn's disease, inflammation can occur across all layers of the bowel wall, which can lead to wall edema, strictures, obstruction, perforation, fistulas, and anal fissures. Inflammation occurs discontinuously and can also manifest symptoms outside the gastrointestinal tract, such as in the skin and joints.
About 20-30% of cases occur in childhood and adolescence, with the highest incidence between the ages of 15 and 35. Onset during childhood and adolescence can impair growth. Additionally, Crohn's disease is characterized by poor wound healing in cases of fistulas or anal fissures, including at surgical sites.